Medical Disclaimer: This article is for informational and educational purposes only and does not constitute medical advice. Diabetic foot complications can be serious and even life-threatening. Always follow the guidance of your physician, podiatrist, or certified diabetes educator for your specific situation. If you notice signs of infection, non-healing wounds, or significant color or temperature changes in your feet, seek medical care promptly.
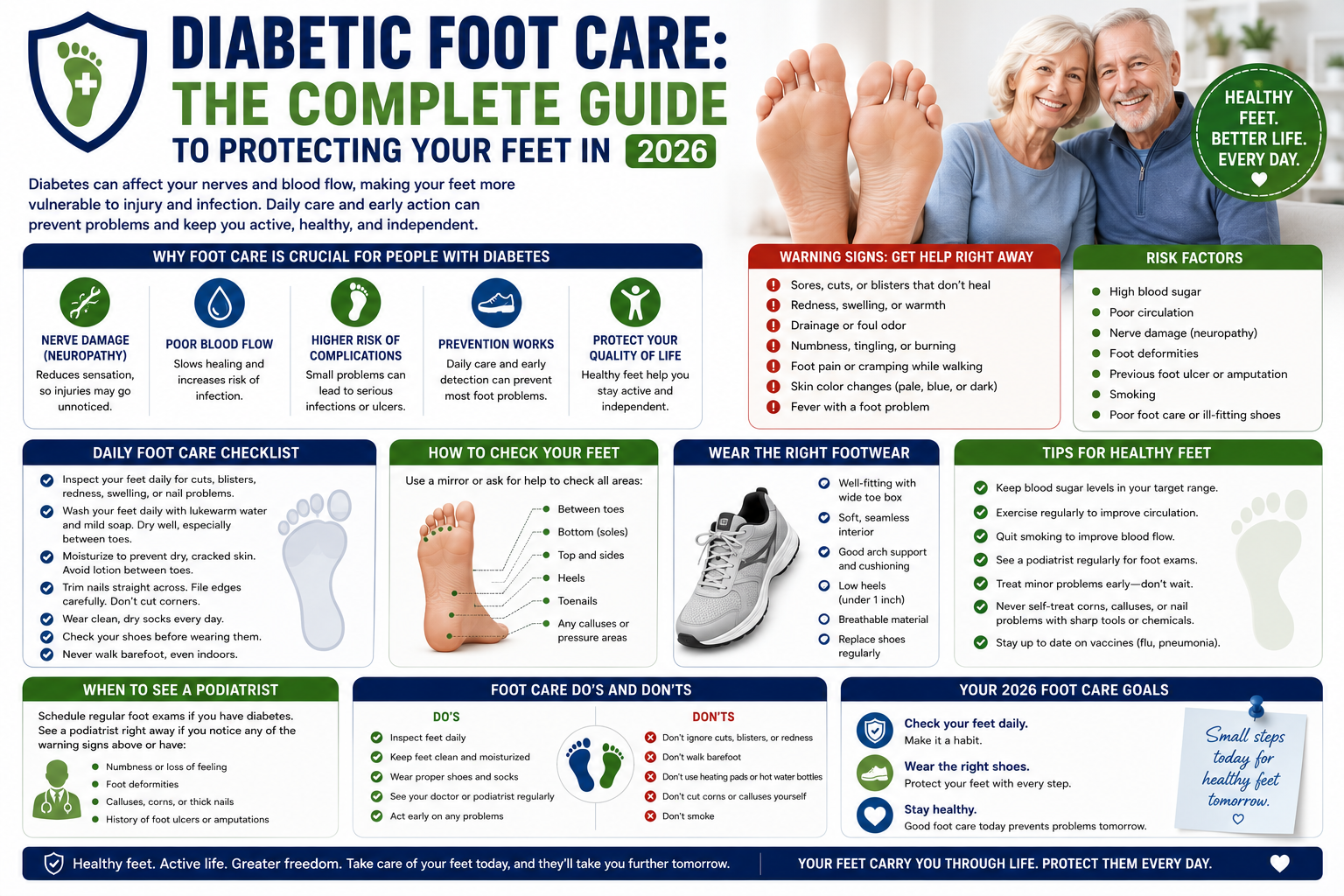
Diabetic Foot Care: The Complete 2026 Guide to Protecting Your Feet
Robert's Wake-Up Call
Robert, 61, had managed Type 2 diabetes for nine years with relative success — his A1C hovered around 7.2%, he took his metformin faithfully, and he exercised three times a week. What he didn't do, until his podiatrist appointment three years ago, was look at the bottoms of his feet. That appointment revealed a small, painless ulcer on his left heel — one he'd had no idea was there. The reason he hadn't felt it? Peripheral neuropathy, the nerve damage that affects 50% or more of people with long-standing diabetes, had quietly reduced sensation in his feet to the point where he couldn't feel a wound that had been there for weeks.
Robert's story is common, and it ended well: the ulcer was caught early, treated with proper wound care and offloading, and healed without complication. But the same scenario, caught later, can lead to infection, osteomyelitis (bone infection), and in severe cases, amputation. The United States sees approximately 130,000 lower extremity amputations annually — the majority diabetes-related, and the majority preventable with proper foot care practices.
This guide covers everything you need to know to protect your feet when you have diabetes: the daily inspection routine, the right products, footwear principles, and the warning signs that require prompt medical attention. When you're ready to stock up on diabetic foot care supplies, AllCare Store carries a full selection of diabetic socks, foot creams, and wound care essentials with free shipping on qualifying orders.
Why Diabetes Is So Hard on Feet
Two interconnected complications of diabetes make feet uniquely vulnerable:
Peripheral Neuropathy: The Silent Danger
High blood glucose over time damages the small blood vessels supplying peripheral nerves, causing progressive loss of sensation, particularly in the feet and lower legs. This "glove-and-stocking" pattern of neuropathy means that by the time it's clinically significant, patients often can't feel pain, pressure, heat, or the presence of foreign objects (a pebble in a shoe, a blister forming) that would normally prompt attention and behavior change.
Neuropathy also affects the small muscles of the feet, contributing to toe deformities (hammertoes, claw toes) and altered gait mechanics that create abnormal pressure points — exactly the spots where calluses form, calluses break down, and ulcers begin.
Peripheral Arterial Disease: The Healing Problem
Diabetes accelerates atherosclerosis in the arteries of the legs and feet, reducing blood flow. Reduced circulation means wounds heal more slowly, infection-fighting immune cells reach injuries less efficiently, and the tissues are less tolerant of pressure and trauma. The combination of neuropathy (can't feel damage happening) and PAD (can't heal damage once it occurs) is what makes diabetic foot wounds so dangerous.
The Daily Diabetic Foot Inspection: Your Most Important Habit
Daily foot inspection is the single most evidence-supported intervention for preventing diabetic foot complications. It should become as automatic as brushing your teeth.
What to Check Every Day
- The tops and sides of both feet — look for blisters, cuts, redness, or swelling
- The soles — use a mirror on the floor or ask a family member if you cannot bend to see clearly; check for calluses, blisters, wounds, or discoloration
- Between all toes — a common site for skin breakdown, athlete's foot, and moisture-related maceration
- The heels — one of the highest-pressure areas; look for cracks (fissures) and any developing pressure wounds
- The nails — ingrown edges, fungal thickening, or discoloration under the nail
- Skin temperature — compare left to right; one foot significantly warmer than the other can signal infection or Charcot arthropathy (a serious diabetic bone complication)
Do this in good lighting, at the same time each day. If you notice anything new or abnormal, don't wait for it to get better on its own — contact your care team.
Daily Foot Washing and Moisturizing
Washing
Wash feet daily with mild, fragrance-free soap and warm (not hot — test water temperature with your elbow or a thermometer, ideally 90–95°F) water. Don't soak feet for extended periods, as prolonged soaking softens the skin and increases vulnerability to breakdown. Dry thoroughly between the toes — fungal infections thrive in damp inter-digital spaces and can create entry points for bacteria.
Moisturizing
Diabetic skin tends to be drier than average due to autonomic neuropathy (which reduces sweating) and impaired skin barrier function. Dry skin cracks, and cracks create open wounds. Apply a diabetic-specific foot cream or thick lotion to the tops and bottoms of both feet after washing — but not between the toes, where excess moisture can promote fungal growth.
Ingredients to look for in diabetic foot creams:
- Urea (10–25%): Softens thick, dry, callused skin; helps prevent fissuring
- Shea butter or cocoa butter: Rich emollients that restore suppleness
- Glycerin: Humectant that draws moisture into the skin
- Tea tree oil (low concentration): Mild antifungal properties for prevention
- Aloe vera: Soothing and anti-inflammatory for dry, irritated skin
Avoid creams with high alcohol content, strong fragrances, or keratolytic concentrations beyond what's recommended for daily use, which can over-thin already-vulnerable skin.
Diabetic Socks: Why They Matter and What to Look For
Standard socks with tight elastic bands, rough seams, and synthetic materials that trap moisture are genuinely problematic for people with diabetes. Diabetic socks are specifically engineered to address each of these issues.
Key Features of Quality Diabetic Socks
| Feature | Why It Matters for Diabetic Feet |
|---|---|
| Non-binding, non-elastic tops | Elastic bands restrict circulation — already compromised in diabetes |
| Seamless or flat-knit toe seams | Traditional seams create friction points that can blister and ulcerate |
| Moisture-wicking fibers (bamboo, merino, CoolMax) | Keeps feet dry, reducing fungal and bacterial growth risk |
| Padded soles | Extra cushioning reduces pressure at high-risk areas (ball of foot, heel) |
| White or light-colored lining | Makes it easier to notice drainage or bleeding from wounds |
| Antimicrobial treatment | Reduces odor and inhibits bacterial/fungal growth |
Browse AllCare Store's Diabetic Socks collection for seamless, non-binding options in a range of styles and materials. We carry brands including Jobst, Silipos, and Dr. Comfort — designed with podiatrist input for maximum protection.
Diabetic Footwear: The Right Shoe Makes a Real Difference
What to Look for in Diabetic-Friendly Shoes
- Wide, deep toe box: Prevents pressure on toe deformities and reduces blister risk
- Breathable upper material (leather or mesh): Reduces moisture accumulation
- Cushioned, supportive insole: Distributes pressure more evenly across the sole
- Low, stable heel: Reduces pressure differential between forefoot and heel
- Adjustable closures (Velcro or laces, not slip-ons): Allows fitting to feet that may swell during the day
- No internal seams or rough edges: Any friction point is a wound risk for neuropathic feet
Medicare-Covered Therapeutic Footwear
Medicare Part B covers therapeutic footwear and inserts for people with diabetes who meet clinical criteria — typically one pair of diabetic shoes and up to three pairs of custom inserts annually. This is an underutilized benefit: talk to your podiatrist about whether you qualify. Therapeutic footwear ordered through a qualified supplier must meet specific clinical requirements and be fitted by a trained provider.
What Not to Wear
- Never go barefoot — even indoors, even briefly. A step on a small object you can't feel is all it takes for a wound to begin.
- Avoid sandals and flip-flops that leave the top and sides of the foot unprotected
- Skip high heels — they dramatically increase forefoot pressure
- Don't wear shoes that are even slightly too small — neuropathy means you may not notice the pain of a tight shoe until there's already damage
Nail Care for Diabetics
Toenail care is a higher-stakes activity when you have diabetes. The risk with self-care is cutting into surrounding skin — something that might not be felt at all with neuropathy but can quickly become infected.
Safe Nail Care Principles
- Cut nails straight across — never round the edges, which encourages ingrowth
- File rough edges smooth rather than cutting aggressively
- Use good lighting and, if possible, magnification
- Soften nails first by soaking (briefly) or trimming after a shower when nails are softer
- Use proper diabetic nail scissors or clippers with a straight edge — not curved scissors
- If you cannot see your feet clearly, cannot safely handle nail scissors, or have significantly thickened or ingrown nails, see a podiatrist for routine nail care — this is covered by insurance in many cases for diabetic patients
Callus and Corn Management
Calluses are the precursor to many diabetic foot ulcers — they represent areas of high, repetitive pressure, and when they break down, the resulting wound is in exactly the spot with the worst pressure profile. Calluses should be managed proactively but carefully.
Safe approaches: Regular moisturizing with urea-based creams softens calluses gradually. A pumice stone used gently on wet skin can reduce buildup over time. Orthotic insoles that redistribute pressure away from callus-prone areas address the root cause.
Do NOT: Cut or shave calluses at home. Do not use over-the-counter corn removers (salicylic acid pads or liquids) without podiatrist approval — they can cause chemical burns on skin with reduced sensation. Persistent or thick calluses should be managed by a podiatrist using sterile instruments.
Wound Care: What to Do If You Find a Wound
If you find a cut, blister, or sore during your daily inspection:
- Don't ignore it. Any break in skin on a diabetic foot requires prompt attention — do not adopt a "wait and see" approach.
- Gently clean the area with mild soap and clean water. Pat dry.
- Cover with a sterile non-stick dressing — non-adhesive dressings are preferred around neuropathic skin that may tear with adhesive removal. Browse AllCare Store's Wound Care collection for diabetic-appropriate dressings and bandages.
- Offload pressure — avoid walking on the affected foot until assessed. Use crutches if needed.
- Contact your healthcare provider — even small diabetic foot wounds should be evaluated promptly. Don't wait more than 24 hours if there is any redness, warmth, or swelling around the wound.
Warning Signs That Require Immediate Medical Attention
Go to an urgent care facility or emergency room immediately if you notice:
- A wound that is increasing in size, depth, or drainage
- Redness, warmth, or streaking spreading from a wound (signs of cellulitis or spreading infection)
- Pus or foul-smelling discharge from any foot wound
- Black, brown, or gray tissue around or in a wound (potential gangrene)
- One foot significantly more swollen, red, or warm than the other without an obvious cause
- Fever combined with any foot wound or skin change
- A foot that has changed shape suddenly (possible Charcot joint)
Diabetic foot infections can deteriorate rapidly. Err strongly on the side of seeking care early.
Diabetic Foot Care Products at a Glance
| Product Category | Key Features to Look For | Where to Find |
|---|---|---|
| Diabetic socks | Seamless, non-binding, moisture-wicking, padded sole | AllCare Store Diabetic Socks |
| Foot cream / lotion | Urea 10–25%, fragrance-free, no alcohol | AllCare Store Skin Care |
| Wound dressings | Non-adhesive, sterile, moisture-balanced | AllCare Store Wound Care |
| Nail clippers | Straight-edge, long-handle, stainless | AllCare Store Personal Care |
| Diabetic shoes / insoles | Wide toe box, cushioned, adjustable closure | AllCare Store Footwear |
| Blood glucose monitor | Fast read, small sample, memory storage | AllCare Store Glucose Monitors |
Frequently Asked Questions: Diabetic Foot Care
How often should a diabetic person see a podiatrist?
Most people with diabetes should see a podiatrist at least once per year for a comprehensive foot exam, even if they have no current foot problems. Those with existing neuropathy, peripheral arterial disease, previous foot ulcers, or structural deformities should typically be seen every 1–3 months. Medicare covers an annual diabetic foot exam and more frequent visits when clinically indicated. Your primary care provider can provide a referral.
Can I use regular lotion on my diabetic feet?
Standard lotions can be used, but diabetic-specific foot creams are preferred because they are typically formulated with higher concentrations of urea or lactic acid to address the thicker, drier skin that accompanies neuropathy, are fragrance-free (reducing irritation risk), and are tested to be appropriate for compromised skin. If using a regular lotion, choose a thick, fragrance-free, alcohol-free formula. Apply to the tops and bottoms of both feet, but not between the toes.
Are diabetic socks covered by Medicare or insurance?
Standard diabetic socks are typically not covered by Medicare as a standalone benefit. However, therapeutic diabetic footwear (shoes and custom insoles) is a Medicare Part B benefit for qualifying patients with diabetes. Check with your insurance plan regarding coverage for specific items. Some supplemental plans and Medicaid programs cover more. A podiatrist or certified diabetes educator can help you navigate your specific benefits.
What is the most common cause of diabetic foot ulcers?
The most common cause is the combination of peripheral neuropathy (inability to feel pressure and pain) and mechanical stress — usually from ill-fitting footwear, repetitive walking on callused or high-pressure areas, or minor trauma that goes unnoticed. The wound itself is often not the primary problem; the inability to feel it and change behavior to protect the foot is what allows it to progress. This is why daily inspection, proper footwear, and regular podiatry care are so effective at prevention.
Is it safe to use a foot spa or pedicure tools if I have diabetes?
Foot spas and electric foot files should be used with caution or avoided if you have significant neuropathy. The risk with foot spas is water that is too hot (difficult to judge with reduced sensation) causing thermal burns. Electric files can remove too much skin. Standard pedicure salons carry infection risk from shared equipment. If you want pedicure-style foot care, it is safest to get it done by a podiatrist or a licensed nail technician who is experienced with diabetic clients and uses properly sterilized instruments. Communicate your diabetes diagnosis before any foot treatment.
Building Your Diabetic Foot Care Routine
Robert now checks his feet every evening before bed — a hand mirror on the bathroom floor, two minutes of careful inspection, followed by his urea cream applied to the soles and tops of both feet. He wears diabetic socks every day and replaced his old shoes with a properly fitted pair recommended by his podiatrist. He's had no recurrence of the ulcer that prompted the change, and his podiatrist tells him his foot health is excellent for someone nine years into his diabetes management.
Two minutes a day and the right products. That's what the evidence supports. And when in doubt — when something looks different, feels different, or just doesn't seem right — the right answer is always to call your care team rather than wait.
Shop AllCare Store's Diabetic Care collection for diabetic socks, foot creams, glucose monitors, and wound care supplies — everything you need for a complete foot care routine. Free shipping on qualifying orders. Questions? Call us at 1-888-889-6260 or visit AllCareStore.com.
— The AllCare Store Team